The Bone Broth Betrayal

The Hidden Histamine Factory in Your Bone Broth — And the Fix Nobody's Talking About
TL;DR
- Most "histamine-safe" diet lists eliminated bone broth based on a preparation error — one that's entirely correctable, and this issue includes the exact protocol to do it
- The histamine doesn't come from the food itself; it's generated by bacterial activity during slow, low-temperature cooking and gradual cooling
- Broth quality is determined before the heat even comes on — sourcing, bone-to-connective-tissue ratio, and cold chain management are the variables most people get wrong
- No correctly prepared broth can ever be "zero histamine" — and it doesn't need to be; the goal is to stay below your personal symptom threshold, not achieve the impossible
- DAO enzyme supplements are a downstream band-aid; the upstream causes of poor histamine clearance require identification through functional lab testing
- HTMA, Organic Acids Testing, and GI-MAP together reveal the mineral, cofactor, and gut-terrain picture that explains why your clearance capacity is compromised
- The ARL HTMA / Video Analysis Bundle is available now at $225 — full mineral analysis with a video walkthrough of every marker on the test
Most "histamine-safe" diet lists are built on a foundational error: they treat bone broth as a dangerous variable rather than a powerful, correctable tool. You don't need to eliminate broth — you need to change your physics.
When the Fix Becomes the Problem
Welcome back to the Rabbit Hole.
Here's how bad information travels in health communities: it starts as a reasonable precaution, gets endorsed by a few trusted voices, circulates widely, and eventually becomes the accepted protocol. Once it's there, almost nobody examines it. The original reasoning gets buried under layers of repetition.
Bone broth got caught in exactly this trap.
Inside histamine-intolerance and MCAS (Mast Cell Activation Syndrome) communities, the guidance spread: bone broth is dangerous. It triggers reactions. Eliminate it. Thousands of people complied. They removed a collagen-rich substrate with genuine therapeutic relevance to gut-barrier repair — glycine and proline derived from collagen hydrolysis do support tight junction synthesis — and replaced it with nothing, usually. Or worse, a collagen powder — a heavily processed substitute that delivers a fraction of the therapeutic payload and carries its own sourcing and manufacturing concerns
The food was not the problem. The preparation method was the problem. And the community institutionalized the error instead of correcting it.
This is what happens when you treat symptoms instead of investigating causes. The solution gets discarded along with the risk.

What's Actually Generating the Histamine
The mechanism is not mysterious once you understand the biochemistry.
Raw meat and bone carry bacteria naturally — that's not a problem under normal circumstances. The problem starts when you cook low and slow. At sub-boiling temperatures (under 212°F / 100°C), those bacteria stay active throughout the entire cooking and cooling process, and they produce histamine the whole time. A broth that has been sitting at 176°F (80°C) for 20 hours isn't a healing food. It's a bacterial incubator that happens to contain collagen.
The cooling phase compounds the problem. The 104–140°F (40–60°C) temperature range during gradual cooling is where secondary histamine generation accelerates. Slow-cooling a protein broth on the stovetop is the biological equivalent of leaving a petri dish at room temperature overnight. The bacteria don't know they're in a wellness recipe.
This is the clinical distinction that most elimination-diet frameworks are structurally incapable of making. The issue was never the food. It was always the methodology. When you remove the food, you remove the therapeutic benefit along with the risk. The correct intervention is to fix the protocol, not eliminate the ingredient.
A Note on Histamine 'Zero'
Let's be clear-eyed about the physics before moving on.
No food containing protein can ever be "zero histamine." Histamine is a naturally occurring byproduct of protein metabolism — it exists in living tissue, full stop. The goal of this protocol is not the impossible standard of zero, which would require eating sterile, synthetic elemental diets. The goal is to drop your total histamine load below your individual threshold — the point at which symptoms begin.
To understand why that threshold exists, it helps to know that histamine clearance in the body runs through two distinct pathways — not one — and this is where most popular explanations quietly fall short.
The first is luminal clearance. This is the domain of DAO, which operates in the gut itself — specifically the upper small intestine — degrading dietary histamine before it can cross the intestinal wall into circulation. Think of DAO as customs at the border: when it's functioning well, most incoming dietary histamine gets intercepted at the gate before it ever enters the system. It isn't reducing the load. It's stopping the import.
The second is intracellular clearance. This is handled by a different enzyme entirely — Histamine N-Methyltransferase (HNMT) — which works inside cells and in systemic circulation, primarily in the liver, kidneys, and central nervous system. HNMT handles histamine that has already crossed the intestinal barrier. Think of it as the domestic police force: it manages what has already entered the country.
These two systems are not redundant. They are sequential and spatially distinct. Compromise DAO — the border agent — and excessive histamine floods into circulation, overwhelming HNMT's capacity to handle the overflow. Compromise methylation capacity — through inadequate B12, folate, or SAM, the methyl donor HNMT depends on — and intracellular clearance falters regardless of how carefully you manage your diet.
Managing diet alone addresses one half of one pathway. This is why elimination diets have a ceiling — and why people who've been meticulously compliant for months still react.
High-heat cooking doesn't destroy every molecule of histamine in raw bone. What it eliminates is the post-slaughter accumulation generated during a 24-hour slow-cook cycle — the bacterial histamine factory that low-temperature simmering enables. By shutting that factory down, we limit the histamine content of your broth to the minimal baseline present in fresh tissue. For most people managing histamine intolerance, that baseline stays comfortably within the tolerable range.
Your Mast Cells Aren't Broken. They're Reporting.
Before we move to the testing picture, there's a framing correction worth making — because it changes how you interpret symptoms entirely.
The standard explanation positions mast cells as immune cells that "overreact" — the central troublemakers of MCAS and histamine intolerance. This framing is incomplete, and it's clinically counterproductive because it frames a measurement as a malfunction.
Mast cells are strategically positioned at every interface between your body and its environment: gut mucosa, skin, airways, blood vessel walls. They are sentinel cells — continuously monitoring local conditions for signals of threat or resource scarcity. When they detect a problem, they degranulate: they release histamine and other inflammatory signals as an alarm.
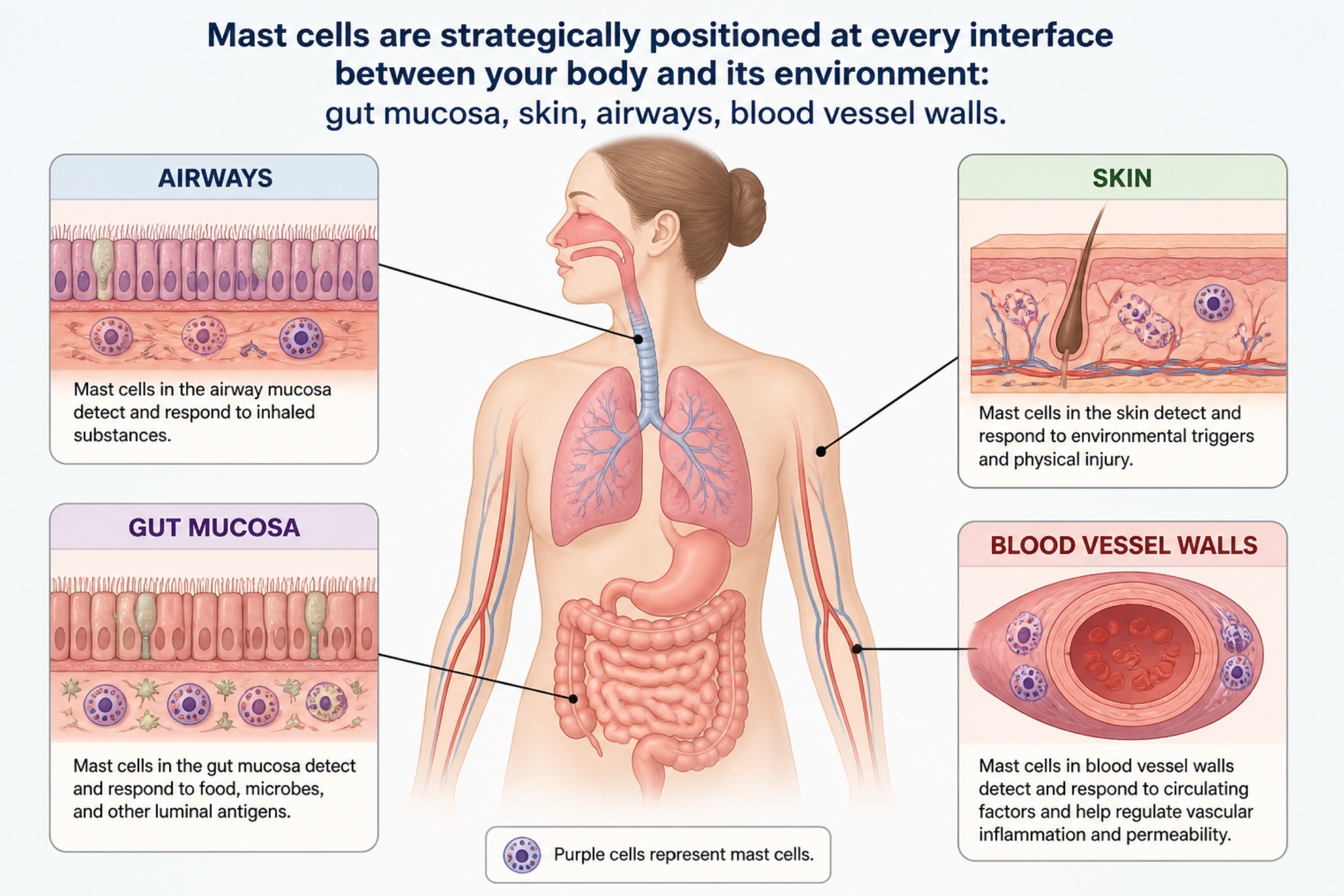
The part most explanations miss is this: mast cells don't degranulate only in response to immunological threats. They degranulate in response to mitochondrial stress, energy depletion, and mineral transport failure. And critically — the threshold at which they fire is not fixed. It drops in direct proportion to the bioenergetic state of the cell. A body under chronic metabolic stress — from oxidative burden, mineral depletion, or poor mitochondrial output — is a body in which mast cells are operating on a failing power supply.
Think of it as a building's security system running on a backup generator that's slowly losing charge. At full power, the alarms are calibrated — they fire on genuine threats. As the power drops, the sensitivity climbs. Inputs that would never have registered at full capacity start triggering alarms constantly. The system isn't broken. It's reporting accurately on a deteriorating energy environment.
In practical terms: if your mast cells are reactive, the question isn't only what you're eating. It's what state your mitochondria are in. What your mineral cofactor levels look like. What your oxidative burden is. These aren't philosophical considerations — they're measurable variables. And this is precisely where functional lab data does its most important work.
Why the DAO Supplement Isn't Solving Your Problem
Here's where a lot of people land after discovering histamine intolerance: they add a diamine oxidase (DAO) enzyme supplement before meals, notice some improvement, and conclude they've addressed the problem. They haven't. They've managed it.
DAO is the primary enzyme responsible for breaking down dietary histamine in the gut. When it's functioning well, histamine from food gets degraded before it can trigger a reaction. When DAO activity is compromised, even modest histamine loads cause outsized responses. Supplemental DAO — typically derived from pea sprouts — works in the gut lumen to degrade incoming dietary histamine. It can reduce symptoms in the short term.
What it doesn't do is answer the more important question: why is your body's own DAO capacity compromised in the first place?

DAO is a copper-containing enzyme. It requires copper as a direct structural cofactor to function. It also requires Vitamin B6 (specifically its active form, pyridoxal-5-phosphate) for enzymatic activity, and adequate zinc status plays a role in the copper-zinc balance that governs both DAO function and broader enzyme metabolism. Beyond the cofactor picture, DAO is produced by the intestinal epithelial cells themselves — meaning gut barrier integrity is directly upstream of your clearance capacity. A compromised mucosal lining produces less DAO regardless of how many supplements you add. And in the presence of significant dysbiosis — including histamine-producing bacterial overgrowth — the rate of histamine generation in the gut can simply outpace what any supplemental enzyme can clear.
Taking a DAO supplement without investigating these upstream variables is the equivalent of putting a trash can under a leaking roof rather than fixing the hole. The trash can catches something. The roof is still leaking.
What the Testing Actually Reveals
This is where functional labs do something standard blood panels cannot: they give you a picture of why the system is underperforming rather than simply confirming that it is.
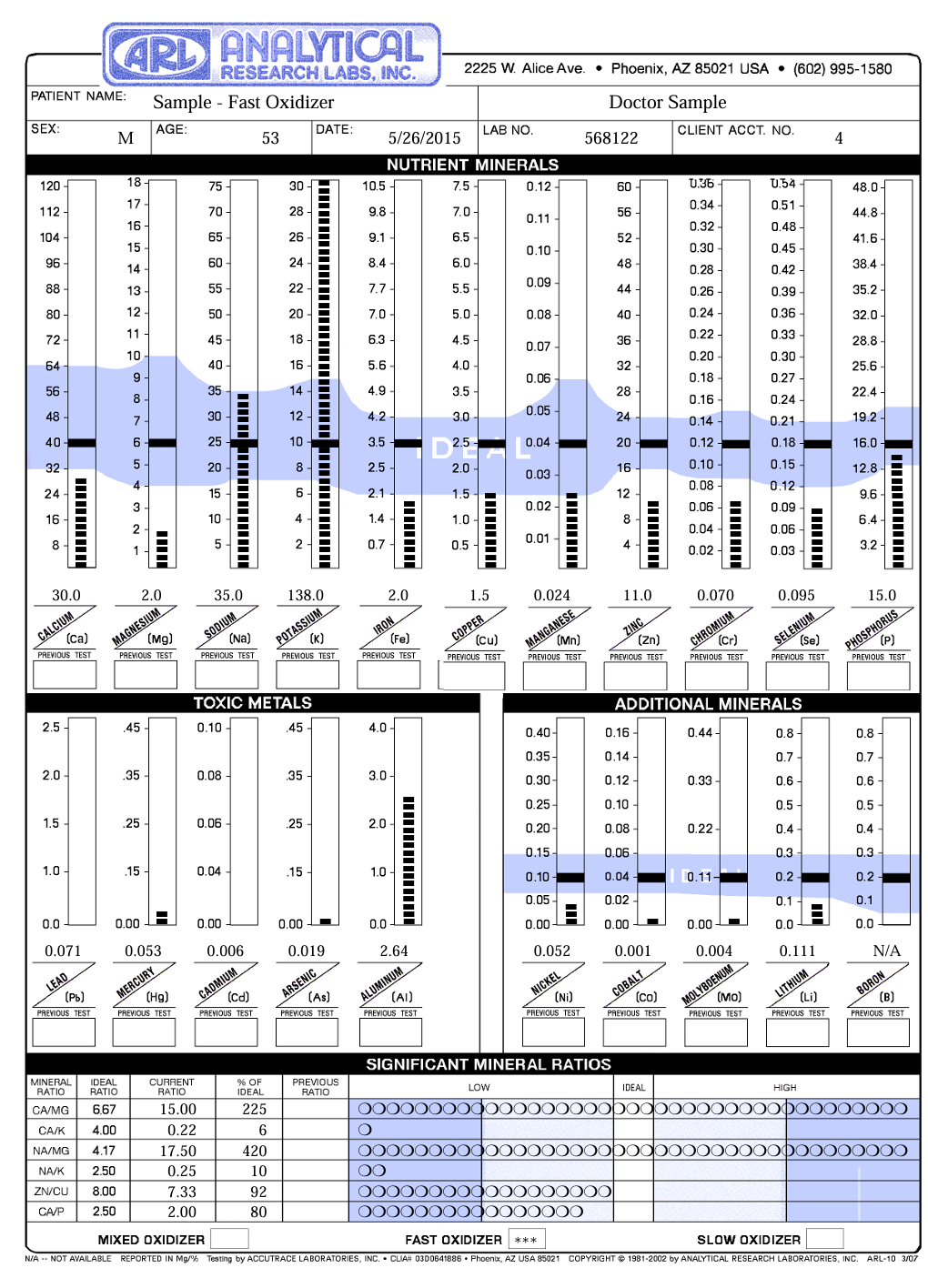
Hair Tissue Mineral Analysis (HTMA) measures mineral status at the tissue level over a 2–3 month window. For histamine and DAO specifically, what it reveals is the mineral cofactor terrain: copper status, zinc-to-copper ratios, magnesium levels, and the broader mineral balance that governs enzyme function throughout the body. Crucially, HTMA does not directly measure Vitamin B6 — B6 is a water-soluble vitamin, not a mineral, and doesn't appear in this panel. That distinction matters, because B6 deficiency is one of the more common and underappreciated drivers of compromised DAO activity.
Start here — and get ahead of what's coming next:
The ARL HTMA / Video Analysis Bundle — available now at $225. A complete Hair Tissue Mineral Analysis, with a pre-recorded video walkthrough of every marker on the test — what each one measures, what the levels mean, and what the patterns reveal about metabolic terrain. This is where the investigation starts. →
SUBJECT: ARL BUNDLE
CONTACT ME
The Histamine Mineral Axis Protocol (HMAP) — This is my forthcoming book that maps the full upstream picture behind histamine dysregulation: the mineral cofactors, the lab patterns, the testing sequence, and the corrective framework that works when elimination diets have plateaued. Newsletter readers get exclusive early access. → [Join the HMAP Early Access Waitlist — Insert Link]
SUBJECT: BOOK WAITLIST
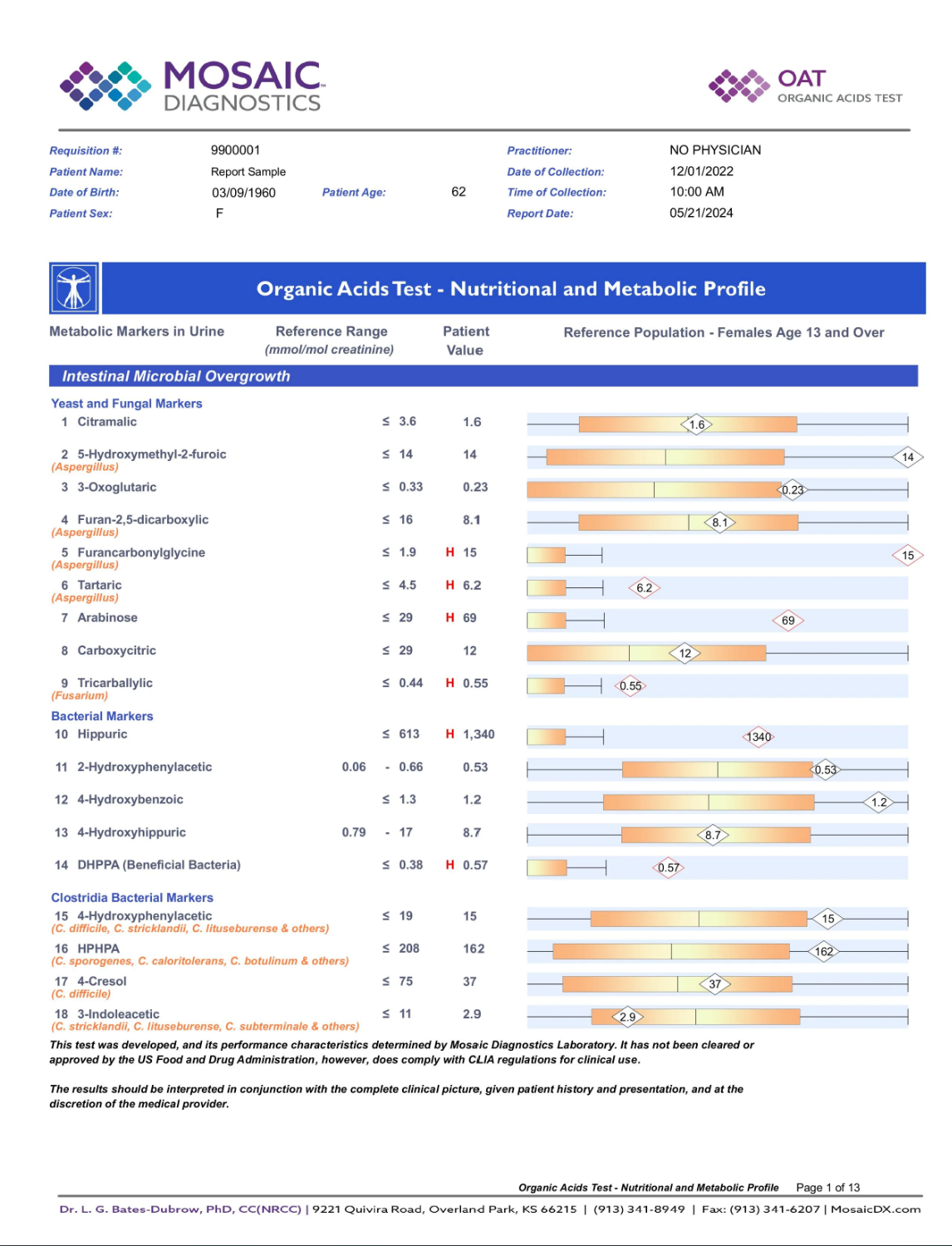
For B6 status, the relevant window is the Organic Acids Test (OAT). When B6 is functionally insufficient, the kynurenine metabolic pathway shifts in ways that produce elevated xanthurenic acid and kynurenic acid in urine — specific organic acid markers that indicate B6-dependent enzyme pathways are under-resourced. In plain terms: when B6 is running low, a metabolic pathway that should be humming along starts producing the wrong chemical byproducts instead. Those byproducts accumulate and spill into urine, where the OAT measures them. It's the body leaving a paper trail of a nutrient shortfall that a standard blood panel won't catch. The OAT also provides a detailed picture of gut dysbiosis through bacterial and yeast metabolite markers, revealing whether histamine-producing microbial overgrowth is contributing to the histamine load independently of what you're eating.
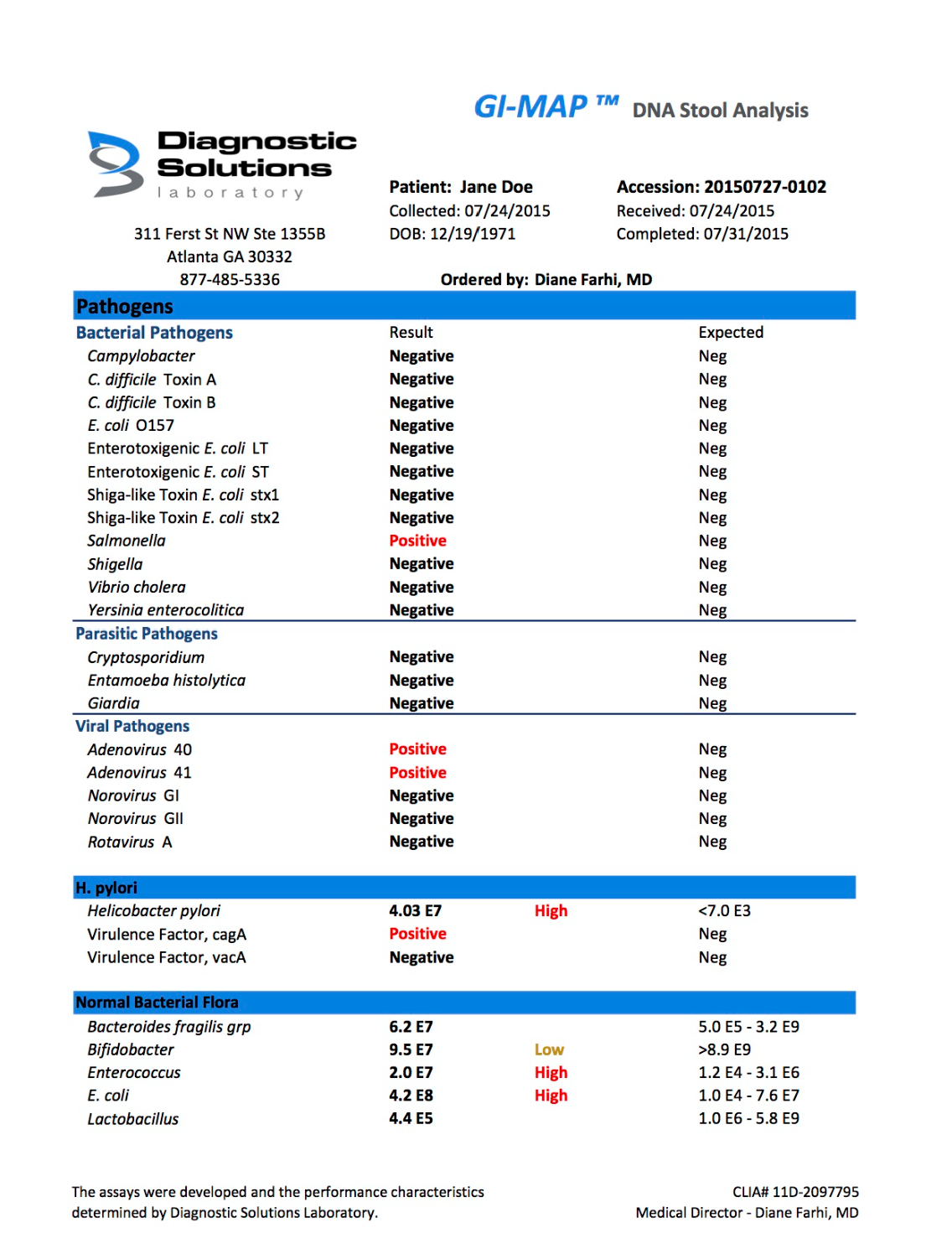
The third piece is GI-MAP, a comprehensive stool analysis that looks at gut barrier integrity directly — secretory IgA (a primary marker of mucosal immune defense), calprotectin (intestinal inflammation), and the microbial landscape including pathogens and commensal organisms — the resident microbes that co-exist in balance with your gut environment under healthy conditions, some of which become significant histamine producers when that balance shifts — associated with histamine production.
No single test tells the complete story. Taken together, HTMA, OAT, and GI-MAP answer the question that a DAO supplement never can: which specific upstream failures are driving your inadequate histamine clearance? From that picture, you can build a targeted protocol — not another round of educated guessing.
The Overton Window in Your Gut Healing Protocol
Zoom out for a moment.
The bone broth error is a microcosm of a larger pattern that runs through health communities — including the most rigorous and evidence-respecting ones. A framework develops, circulates, gains authority, and eventually contains institutionalized errors that nobody is actively questioning because the framework itself has become the accepted standard of care.

RECIPE: THE ULTIMATE QUICK COOK BONE BROTH - Histamine Safe!
🔬 Protocol Note: The Broth Architecture
A note before we get into the method: this preparation protocol isn't only for people managing histamine intolerance. It's the right way to make bone broth for anyone. There is no good reason to introduce an unnecessary histamine burden into a healthy system, and every reason to produce the most nutrient-dense, therapeutically complete broth possible. The protocol below is the standard — not a workaround.
The quality of your broth is determined before the heat comes on. It is a function of sourcing, ratio, and how you've managed the cold chain.
Part One — The Architecture: What Goes In
The 50/50 Ratio To produce a gelatinous, nutrient-dense broth, you need to balance two distinct structural requirements. The standard protocol is a 50/50 mix by weight:50% Marrow Bones — the scaffolding. This is your mineral density.50% Connective Tissue — knuckle bones, feet (chicken, pork, or beef), neck bones, or trachea. This is the mortar. It provides the glycine and proline-rich collagen your gut epithelium requires to seal tight junctions. This is the therapeutic payload. Don't shortchange it.
The Sourcing Hierarchy Do not default to generic grocery-store "soup bones," which are often poor-quality remnants with compromised fat profiles. Work down this list:The direct butcher relationship — Call a local independent butcher. Ask specifically for knuckle, feet, and neck bones. These are undervalued cuts, often sold for a fraction of premium prices. A recurring order here is the most cost-effective, high-quality path available to most people.Regenerative online sources — For those who prioritize time over local sourcing: US Wellness Meats and White Oak Pastures offer pre-portioned broth kits that approximate the required 50/50 ratio without manual sorting.
The Cold-Chain Requirement Treat your bones with the same standard as your steaks. Bones stored in a freezer for months undergo lipid oxidation — the fat profile degrades, and rancid oxidative byproducts end up in your broth. Purchase bones in bulk, portion them immediately into 50/50 ratio bags, and freeze. Move from freezer to cooker directly. If the marrow is discolored or the fat shows freezer burn, the structural lipids are already compromised. Do not use them.
Part Two — The Method: How It Gets Made
Step 1 — Correct the water ratio. The most common complaint about this method is that the broth tastes thin. This is a concentration problem, not a time problem. The richness of a long-simmered broth comes from water evaporation concentrating the dissolved collagen, fat, and minerals — not from the hours themselves. Use the minimum water required to cover the bones — typically no more than 1 to 1.5 litres per kilogram of bone. A correctly prepared broth sets to a firm gel when refrigerated. If it remains liquid, the ratio was too dilute.
Step 2 — Cook at high heat, not low and slow. 90 to 120 minutes at high temperature is sufficient to extract collagen from most connective tissue cuts, and critically, eliminates the bacterial activity that drives histamine accumulation during prolonged low-temperature cooking. Time is not your friend here. Heat is.
Step 3 — Rapid cooling is non-negotiable. Transfer immediately to an ice bath. Do not allow the broth to pass through the 104–140°F (40–60°C) range slowly — this is where secondary histamine generation compounds during gradual cooling. Cool rapidly, then refrigerate immediately.
Step 4 — Finish with purpose. Before drinking, whisk in a knob of high-quality grass-fed butter and a pinch of unrefined sea salt. Grass-fed butter contributes short- and medium-chain saturated fatty acids that support mitochondrial membrane integrity and provide an immediate fat-oxidation substrate. Unrefined sea salt contributes trace mineral cofactors — including the magnesium and potassium relevant to cellular ion transport — systematically absent from most elimination diets. The emulsified fat also improves satiety signaling significantly through cholecystokinin release, which matters for anyone whose appetite cues have been disrupted by months of inadequate caloric density.
Optional flavor additions: Fresh ginger root, rosemary, or thyme carry no histamine consequence when added at the start of cooking — provided they are genuinely fresh, not stored for days at room temperature. Ginger's gingerol compounds carry independent mast-cell-stabilizing properties, making this a functionally useful addition rather than merely cosmetic. Avoid any aged, dried, or fermented flavoring additives — miso, soy-based pastes, aged vinegars, pre-made stock concentrates. These reintroduce the exact histamine load the preparation correction was designed to eliminate.
Watery broth means the concentration ratio was wrong. Bland broth means the fat and mineral integration was skipped. Neither problem requires more cooking time. Both have immediate, mechanistic solutions.
Stop thinking like a chef. Start thinking like a biochemist building a fuel source.
A note on equipment.
A slow cooker or crock pot — even one with a locking lid — is not a substitute for high-heat cooking. A locking lid creates a steam seal for safety. It does not build pressure, and it does not get hot enough to neutralize bacterial histamine activity. If you've been using one for broth, this is likely a significant part of why it hasn't been working for you.
For high-heat broth production, the two main categories are electric multicookers (the Instant Pot and its equivalents, widely available at $60–$200) and stovetop models, which reach higher temperatures and last longer but require more attention ($70–$280+). In both cases, insist on a stainless steel inner vessel. Avoid aluminum — acidic broth will leach aluminum into the liquid over repeated use — and avoid any non-stick coated pots for the same reason.

It happens in mainstream medicine — where "normal" lab ranges derive from population averages of largely unwell people, and where the acceptable range of health discourse is narrower than most patients realize. But it happens in ancestral and functional health spaces too. Carnivore resolves everything. Keto corrects all metabolic dysfunction. Histamine intolerance means eliminating high-histamine foods indefinitely.
These positions contain real insight. They also contain load-bearing errors that silently block results for a meaningful subset of people — people who often blame themselves for not complying hard enough.
If you've been following the protocol precisely, eliminating correctly, supplementing reasonably, and still reacting — the answer probably isn't to eliminate more things. The answer is to verify what the protocol hasn't examined. You need the actual data on what's happening inside your specific biochemistry before you make another adjustment. The terrain is individual. The interventions need to be too.
Sleuth Wellness: Functional Health for the Real World
The Sleuth Wellness approach is built for people who understand health sovereignty but need a verified map, not another one-size-fits-all protocol. If you've cycled through elimination diets, carnivore, keto, and DAO supplements and still can't get ahead of your symptoms — the missing piece is almost always upstream data you don't have yet.
Functional lab testing through Sleuth Wellness goes considerably further than anything a standard clinic orders: HTMA for tissue-level mineral and toxic metal status, Organic Acids Testing for cofactor and dysbiosis patterns, GI-MAP for gut barrier and microbiome assessment, DUTCH Complete for hormone and HPA-axis function. The results get mapped against the signals your body is already sending — not to treat the paper, but to build a genuinely personalized protocol around your biology and your actual life.
Don't Trust. Verify.
Standard medicine runs an opaque system. It interprets your data through reference ranges derived from a mostly-unwell population and returns a verdict: "normal." The gap between "you won't die today" and "your systems are actually functioning well" is enormous, and that gap is where most chronic dysfunction quietly lives.
Functional labs are the alternative model — your data, your insights, unfiltered. Not a protocol designed for the average person who doesn't exist. A picture of what's actually happening in your specific body, right now.
For the person who understands the value of verification — who has learned through experience that trusting opaque systems with your most important assets tends to end badly — functional testing isn't a luxury. It's the foundation of an intelligent protocol.
Let not perfect be the enemy of good, but let data replace guessing everywhere it can.
The Takeaway
Bone broth belongs in your healing protocol. The preparation method most people use does not.
The error was never about the food. It was about the physics — prolonged low-temperature cooking and slow cooling creating conditions where bacterial histamine generation compounds with every passing hour. Fix the physics and you recover one of the more genuinely therapeutic preparations available: a collagen-dense, mineral-rich, fat-integrated fuel source that supports gut-barrier repair, mitochondrial function, and satiety signaling simultaneously.
Understand the error and you understand something larger. The health frameworks we inherit — even from rigorous, evidence-respecting communities — can contain institutionalized mistakes that nobody is currently examining. The most important skill in health optimization isn't compliance with a protocol. It's the willingness to ask whether the protocol has examined its own assumptions.
That question never stops being worth asking.
| |||||||||||||||||||||||
P.S. In future issues, I will be unveiling a "hidden handbrake" diagnostic — a low-friction screening tool to identify toxic heavy metal interference. If your mineral axis remains locked despite dietary correction, this will be your final step toward metabolic resolution.
Note: This newsletter is for educational purposes only and is not intended to diagnose, treat, or cure any medical condition. Always consult with qualified healthcare providers regarding any health concerns.
Let not perfect be the enemy of good.
Rabbit Hole Health is a newsletter by Sleuth Wellness, dedicated to helping sovereignty-minded individuals take control of their health through functional testing, personalized protocols, and verification-based approaches. We respect the ancestral health pioneers while acknowledging that not everyone fits the "perfect maxi" mold — and that's okay.
Want to go deeper down the rabbit hole? Reply to this email or visit sleuthwellness.com to learn more about functional testing options.



